Most people have never heard the word allogeneic until someone they care about gets sick. It sounds like something from a medical textbook you’d close after two pages. But the idea behind an allogeneic stem cell transplant is actually pretty simple.
It means the stem cells come from someone else. That someone could be a sibling, a parent, or a total stranger on the other side of the world who joined the registry years ago and never expected to hear back. For the patient, it can be the difference between running out of options and getting a real shot at recovery.

Trace Richey during his allogeneic stem cell transplant at St Vincent’s Hospital.
Why an allogeneic stem cell transplant is needed
Blood cancers and serious blood disorders can wreck the bone marrow to the point where it stops making healthy blood cells. When that happens, the body can’t fight infections, carry oxygen properly, or stop bleeding the way it should.
Chemotherapy can sometimes get the disease under control. When it can’t, doctors look at a stem cell transplant. If they can’t use the patient’s own stem cells, they need someone else’s. That’s when doctors consider an allogeneic stem cell transplant.
The donor’s stem cells travel to the patient’s bone marrow and start building a brand new immune system from scratch. It’s not a blood transfusion. It’s more like a full reset.
How matching works
This is the bit that surprises most people. Matching isn’t about blood type. It’s about tissue type.
Everyone carries a set of markers on their cells called Human Leukocyte Antigens, or HLA markers. You get half from each parent. These markers are basically your immune system’s ID. When someone needs a transplant, doctors look for a donor whose HLA markers line up as closely as possible with the patient’s.
A close match means the new stem cells have the best chance of doing their job without the patient’s body fighting them off, and without the donor’s cells reacting against the patient’s tissues. That second one is called graft versus host disease, and a better match helps lower the risk.
Siblings have roughly a one in four chance of being a full match. Another good reason to be nice to them. When that doesn’t work out, doctors search the Australian and international registries for an unrelated donor. We’ve explained how that search actually works if you want the full picture.
What the donor actually goes through
Most donations in Australia happen through the blood, not the bone marrow. Around 90 percent of stem cell donations use a method called peripheral blood stem cell collection, or PBSC.
In the days before donation, the donor has daily injections of a medication called G-CSF. It tells the bone marrow to go into overdrive, creating more stem cells which end up in the bloodstream, making it much easier to collect. On donation day, the donor sits in a chair while a machine filters the stem cells from their blood and returns everything else. Five to six hours, no surgery, no general anaesthetic. It’s just like a long plasma donation. Most donors spend it watching Netflix and wondering what the fuss was about.
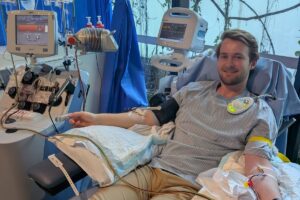
Hunter on stem cell donation day at the Kinghorn Cancer Centre.
In the remaining 10 percent of cases, doctors collect stem cells from the bone marrow under general anaesthetic. They only go this route when it gives the patient a better outcome. The donor might feel sore for a few days, but it settles quickly.
Either way, the donor always has the final say. No one donates without being fully informed and fully willing. If you want to know exactly what donation day feels like, we’ve covered what really happens to your body when you donate stem cells.
What happens on the patient’s side
Before the transplant, the patient goes through high dose chemotherapy and sometimes radiation. This clears out the damaged cells and makes room for the new ones to take hold.
The donated stem cells go in through a drip, similar to a blood transfusion. Once inside the body, they find their way to the bone marrow and start producing healthy blood cells again. This part is called engraftment, and it usually takes a few weeks.
During that time, the patient stays in hospital with a medical team watching everything closely. Their immune system is essentially starting over, so even a small infection can be serious. Recovery after an allogeneic transplant is slow and hard work. But many patients go on to live long, healthy lives because someone else’s stem cells gave their body the chance to rebuild.
Why more young Australians need to join the registry
More than a thousand Australians need a stem cell transplant each year. Even with that demand, overseas donors still provide over 80 percent of the stem cells used for Australian patients.
You inherit HLA markers from your parents, so the best match often comes from someone with a similar background. That means the registry needs to reflect the mix of people who actually live here. Right now, some communities are well represented and others have very few donors on the list. For patients from those backgrounds, the search takes longer and sometimes leads nowhere.
Every person who joins changes the odds for someone else.
Ready to join the registry?
If you’re aged 18 to 35, in good general health, and have a green or blue Medicare card, you can join the Australian stem cell donor registry. A few minutes online, a cheek swab kit to your door, and you’re on the list.
Most people who sign up will never get the call. But if you do, it means your tissue type is the match someone has been searching for.
Sign up through the TLR Foundation’s partner page.
Be a legend. Save a life.
References
TLR Foundation — Become a stem cell donor
Cancer Australia — Stem cell transplants