When someone needs a stem cell transplant, doctors look for a donor whose tissue type closely matches theirs. That match might come from a sibling or from a stranger on the stem cell donor registry. But sometimes neither works out. The siblings aren’t a match, and no one on the registry is close enough.
That’s where a haploidentical stem cell transplant comes in. It’s usually just called a haplo. Instead of waiting for a perfect match, doctors use a half-matched family member as the donor. A parent, a child, a brother, or a sister. You inherit half your tissue type from each parent, so almost everyone’s got at least one potential haplo donor in their family. When the usual routes don’t deliver, a haplo transplant means treatment doesn’t have to stall.
What does haploidentical mean?
Haploidentical means half-matched. It comes down to tissue type, which is determined by proteins on the surface of your cells called HLA markers. You get half from your mum and half from your dad. Doctors care about these markers because a stem cell transplant isn’t just replacing blood cells. It’s putting a whole new immune system into someone’s body. If the match isn’t close enough, the new immune system can start attacking the patient’s own tissue. Doctors call this graft versus host disease, or GvHD. The closer the match, the lower the risk.
How haplo transplants became a real option
For a long time, doctors wouldn’t go near half-matched donors. The risk of severe GvHD was too high, and outcomes were poor. But over the past two decades, research changed that. Better medications, more precise treatment plans, and closer monitoring after transplant made it possible to use half-matched donors safely. Outcomes improved to the point where haplo transplants now sit alongside fully matched transplants as a genuine treatment pathway.
The numbers back it up. In Australia, haplo and other related donor transplants have been climbing steadily for over a decade and they’re still rising.
Why haplo transplants matter more for some communities
Tissue type is closely linked to ethnic background. Matches are more likely to come from someone with a similar heritage, which means people from diverse or mixed backgrounds often have a much harder time finding a closely matched donor on the registry.
For First Nations Australians, the challenge is different again. The unique genetic diversity of Aboriginal and Torres Strait Islander peoples means overseas registries offer essentially no help. A match almost certainly has to come from within the community, and right now, there aren’t enough First Nations donors on the Australian registry to make that reliable.
In all of these situations, haplo transplants can be the difference between starting treatment and waiting indefinitely. When a family member is half-matched and ready to go, doctors don’t have to keep searching for a donor who may not exist on any registry in the world.
When a family member steps in
Sometimes the best donor is already in the room. Abbey donated her stem cells to her mum Maggie when she needed a haploidentical transplant at the Kinghorn Cancer Centre. They weren’t a full match, but they didn’t need to be. You can read Abbey’s story here.
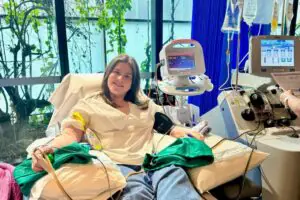
Abbey donating stem cells for her mum
That’s one of the things that makes haplo transplants different. The donor isn’t a stranger on a registry somewhere. It’s someone who already knows the patient, already cares, and is usually ready to go quickly. When time matters, that can make all the difference.
Why the registry still matters
Even with haplo transplants, not everyone’s got a family member who can donate. Some people are only children. Some are estranged from family. In other cases, a parent might be too old or not medically able to go through the process. For plenty of people, a family donor simply isn’t an option.
That’s where the stem cell donor registry becomes critical. It connects patients with unrelated donors who share a close tissue type match, sometimes from the other side of the world. The more people who join, especially young people from diverse backgrounds, the better the odds that someone finds their match in time. You can find out more about how matching works here.
Haplo transplants have expanded what’s possible, but they haven’t replaced the need for a strong and diverse registry. Both matter and that’s where you come in.
Ready to join?
If you’re aged 17 to 35, you can join the registry with a simple cheek swab sent to your door. Most people who sign up will never get the call, but if you do, you could be the reason someone gets to start treatment. Sign up through the TLR Foundation’s partner page.
Be a legend. Save a life.